Minor scrapes and cuts can be easily treated with proper cleansing and bandaging. But when they are more serious, such as a laceration, gash or another type of break in the skin, medical intervention may be required. If so, the doctor will likely use staples or sutures to stitch the wound. Let’s learn more about each of these techniques and how to know which one is appropriate.
Sutures
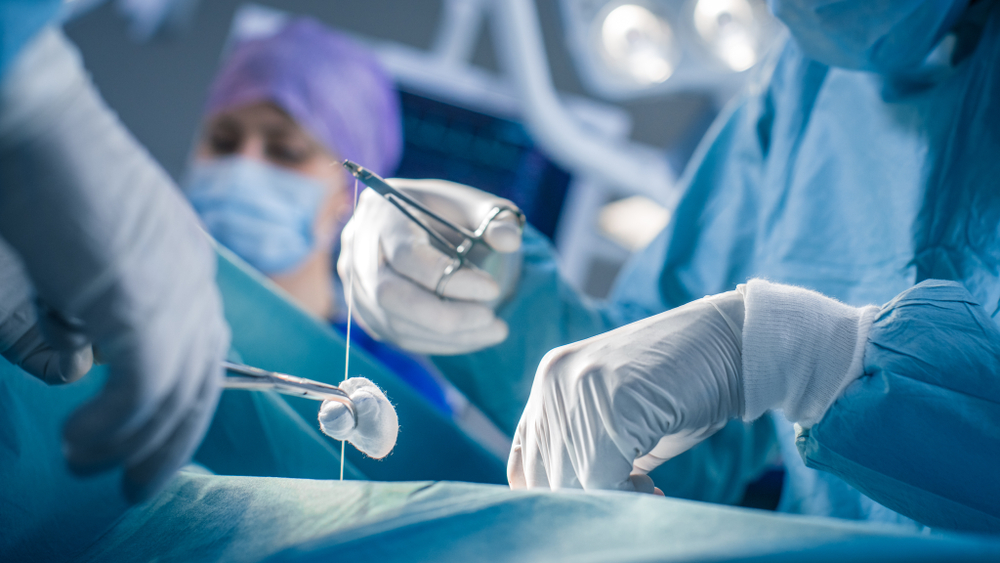
Sutures are the most commonly used choice for skin repair. A suture is simply a piece of thread, like sewing thread, attached to a needle. The needles are of various sizes and have a cutting or non-cutting edge. The doctor will “sew” your skin together just like sewing fabric.
Sutures are classified according to the structure of the thread and where the material comes from. Single-thread sutures are more delicate, making them easier to guide through tissue. Multi-thread or braided sutures make for a stronger closure but can also increase the chance of infection.
Sutures can be continuous, using one thread throughout, or interrupted, using several threads in case one comes out. They are made from natural or synthetic materials.
Finally, sutures will either be permanent and non-absorbable - that is, they remain in your skin until a doctor removes them - or will absorb into your skin and be dissolved by enzymes in your body. Permanent sutures are often used to close surgical incisions or lacerations or simply for wounds that cut through several layers of skin and will require a longer healing time.
Finally, there are many suture techniques. The doctor’s selection depends on the depth and severity of your wound, as well as whether it’s simple outpatient or surgical in nature.
- Purse-string: continuous suture placed around the wounded area and tightened like a drawstring
- Buried: internally placed permanent suture
- Subcutaneous: suture placed just below the upper layer of skin in a line parallel to the wound
- Deep: continuous or interrupted suture place under several layers of tissue
Nonabsorbable sutures
These sutures must be removed by a doctor, usually about two weeks after insertion. In rare cases, they are left in permanently. There are several types of nonabsorbable sutures. They include synthetic single-thread (polypropylene), natural braided thread (silk), natural single-thread (nylon) and synthetic braided thread (polyester). These are most appropriate for neurological and cardiovascular surgery.
Absorbable sutures
These dissolving sutures are generally used for more delicate areas such as inside the mouth, as stitches removal is not required. They can be used for skin grafting, protecting lost or burned skin with healthy skin taken from elsewhere on the body. They are also used for lower layers of skin, connective tissue or muscle and any area with blood vessels just under the skin’s surface. Absorbable sutures come in the following types:
- Polydioxanone (PDS): synthetic single-thread used best on soft tissue and in cardiac procedures for children
- Gut: Natural single-thread that causes a strong reaction and scar; designed primarily for gynecological surgery
- Polyglactin: synthetic braided suture best for hand or face injuries
- Poliglecaprone: synthetic single-thread appropriate for soft tissue repair and to close skin without leaving a scar
Only PDS sutures should be used in neurological or cardiovascular procedures.
Staples
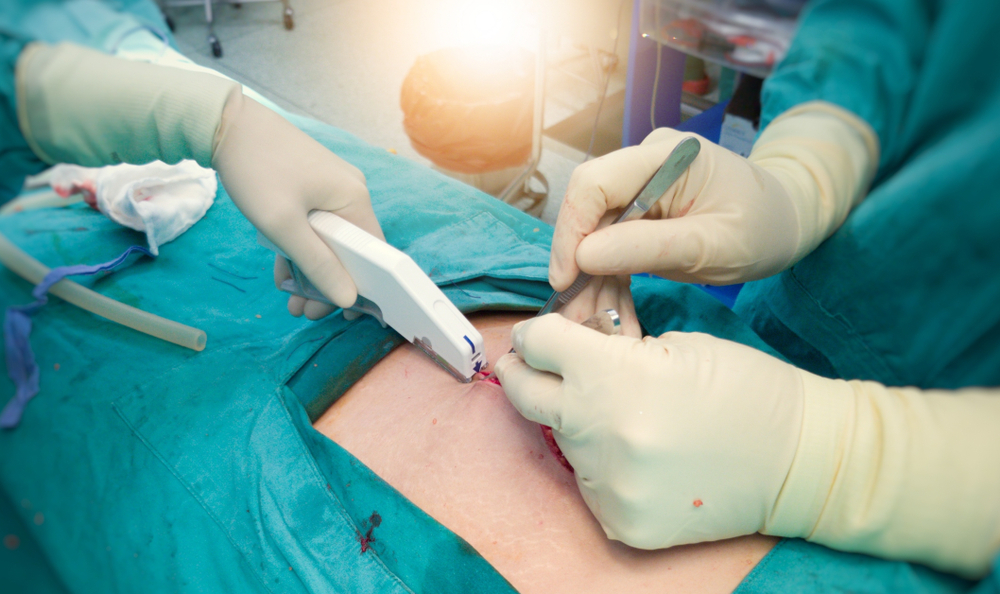
Surgery staples are an alternative to sutures; they are usually non-absorbable and must be removed after a maximum of 21 days. Some stay in permanently for especially damaged tissue or organs. The length of time they must stay in depends on what surgery you had, how severe your wound is and other factors.
Staples are placed with a special wound stapler, which often resembles the larger construction stapler with a lever and handle. All the doctor has to do is correctly maneuver the stapler and push it down. The process is much faster than manually sewing with sutures. Always follow your doctor’s instructions for post-staple care.
Staple removal, which should not be painful, requires special tools and procedures only available through your doctor. For this reason, you should never try to take them out yourself. Here are the steps to removing staples after surgery:
- Remove any bandages, clean the area
- Make sure the wound looks healed and not infected
- Slide part of the surgical staple remover tool under the staples on both ends of the wound, then wiggle it side to side until it comes out
- Repeat the above step on every second staple, then remove the others
- Protect each incision with a steri strip
Surgical staples can be made from a variety of materials depending on the circumstances. Stainless steel can be helpful for patients with metal allergies; titanium if the doctor is concerned about an infection; plastic is readily available and can be good for scar healing, and a biodegradable polylactide-polyglycolide copolymer is great for plastic surgery as it greatly reduces cosmetic damage.
Staples may be the best option when the wound is too big or surgery too complex for sutures. They can also speed up surgery time, lessen pain and reduce infection risk. If you have a C-section, for example, staples will leave less of a scar and shorten your recovery time.
Advantages and Disadvantages of Sutures & Staples
One study comparing sutures v. staples found no satisfactory evidence that produced a clear winner. Researchers evaluated variables such as infection, readmission rate and pain. A physician’s preference is unique to the situation and their experience, but either choice has its pros and cons.
In general, surgical staples produce a faster healing time with less inflammation and easier removal. They are often best for difficult surgeries. Sutures can sometimes be more cosmetically pleasing and only need one doctor to perform, which is ideal for outpatient cases. But while surgical staples have slightly more advantages than sutures, they also carry higher risk.
Risks and Precautions
Regardless of your chosen method, it’s best to take precautions for the best chance at proper healing. Your physician should always keep a good blood supply running to the wound, align the stitches to natural edges in the skin, always use Band-Aids or other sterile wound covers, use the right size and material, and make sure not to over-tighten or over-staple. Failing to do these things can result in complications and injuries ranging from mild to serious, including:
- Infection and early wound opening
- Blood clots or fistulas
- Allergic reactions
- Sepsis or internal bleeding
- Organ damage
What To Do About Surgical Stapler Injuries

You may be surprised to learn that the U.S. Food and Drug Administration (FDA) categorizes surgical staplers with low-risk medical tools like bandages and tongue depressors. But there were 41,000 adverse medical events due to staplers between 2011-2018, and a quarter of those were serious injuries or death. The FDA was underreporting even more incidents and is now considering moving staplers to a higher-risk class.
If you or a loved one has suffered due to negligent surgical stapling, your best path to justice is to consult an attorney knowledgeable in dangerous product personal injury. It’s even better if that attorney has dealt specifically with medical devices and injuries. Take the time to do your research - your peace of mind will thank you.










